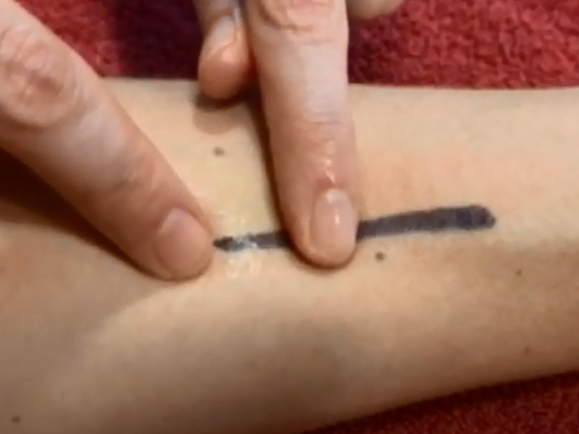
Spotlight on Subcutaneous Mastectomies for Transgender Patients
When we’re talking about mastectomies and post-op recovery, there’s another procedure to highlight in terms of post-mastectomy care. You might hear it called “top” surgery, FTM (female-to-male) or FTN (female-to-nonbinary) top surgery, “chest...